Neuropathy can be difficult to diagnose. It covers many different nerve types, can express itself in several different ways and in different parts of the body.
Diabetic neuropathy can affect individuals who have had diabetes for a long time and is characterised by a loss of tactile perception that can lead to serious foot ulcers and, in the worst cases, to amputation. Approximately one third of all diabietes patients with neuropathy suffer significant pain.
“The pain usually feels like a burning or aching pain in both legs. Other parts of the body can also be affected, although this is less common. The pain is often worse at night”, says Eero Lindholm, researcher at Lund University and consultant at the Endocrinology Clinic at Skåne University Hospital in Malmö.
Vibrations and pressure
To detect nerve damage at an early stage, the feet are therefore regularly examined as part of the diabetes care. During the examination, the patient is tested on their ability to feel vibrations and pressure with different tools.
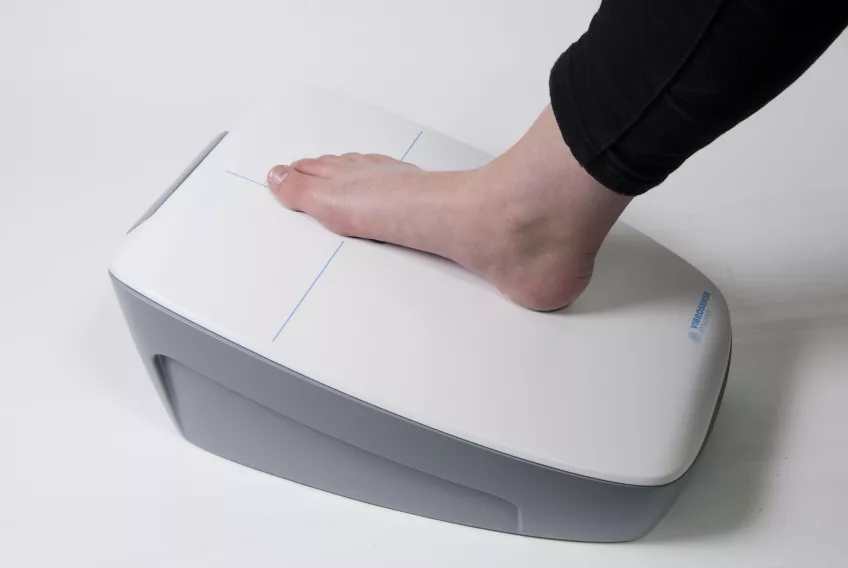
In recent years, Eero Lindholm has studied the nerve sensitivity in the feet of diabetes patients with the help of so-called vibrometry. The patient places their foot on a plate that emits low and high frequency vibrations. The low frequency vibrations are felt like taps that occur four times per second. The high frequency vibrations are emitted 250 times per second.
“It has been demonstrated that it is often the sensitivity to the high frequency vibrations that is lost first. However, the risk of foot ulcers increases if the patient no longer feels the low frequence vibrations. This may be due to the fact that the receptors that are sensitive to low vibrations are also important for balance and are weight-bearing when you walk.”
Unpleasant method
In an ongoing research project, Eero Lindholm and his research colleagues compare the vibrometry results with nerve conduction velocity studies that are carried out with neurography, an examination sometimes used in healthcare to study nerve function. Small electrodes placed on the feet emit electrical signals that register the actual capacity of the nerves. Not all patients appreciate this, instead, they think the method is unpleasant, according to Eero Lindholm. “The method is also time-consuming; it takes approximately 60 minutes.”
Preliminary data shows that the two measurement methods have correlating results, i.e. they coincide to such a high degree that vibrometry, which is a simpler examination and does not cause discomfort, could replace the neurography examination in diabetes patients.
“For it to become a method we can use clinically however, we first need to make it more efficient. A screening should take five-ten minutes, it currently takes 30-45 minutes.”